Fibromyalgia Pain-It’s More Likely for Those with Rheumatic Conditions

Fibromyalgia pain is currently one of the most common types of pain in the world.
It can be debilitating.
The United States currently has more individual diagnoses for fibromyalgia than any other country.
This painful condition, caused by chronic widespread pain can stop you in your tracks.
The joint pain and nerve pain is often tolerated by individuals until they feel they can no longer live with it before they report it to a doctor.
The danger in this is that there are now more medications prescribed for this pain than any other type of pain, and it is often misdiagnosed.
This leaves those who suffer feeling frustrated and discouraged.
The plan of treatment in conventional medicine is to prescribe medication and physical therapy, with no other option.
There are some doctors that have reportedly suggested to their patients to use natural supplementation like fish oil, and glucosamine chondroitin to improve their joint function and improve their overall mobility.
This is good news for those who suffer from painful rheumatic conditions, but those supplements may not be enough long-term.
This article will share how you can potentially identify symptoms of fibromyalgia, what to consider if you have been given a diagnosis for this condition.
You’ll learn more about your options for conquering fibromyalgia pain naturally.
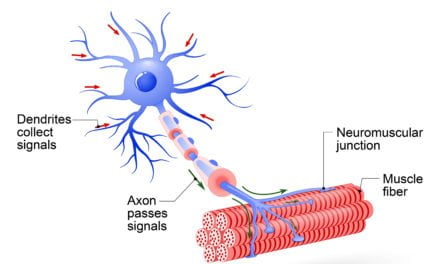
Fibromyalgia Pain-Identify Tender Points
Pain isn’t easy to deal with, especially when it is constant.
Pain isn’t easy to deal with when it’s intermittent, but there are certain signs to look for if you haven’t been diagnosed with fibromyalgia.
It can be beneficial to view a pain chart that correlates with fibromyalgia if you are still unsure about your diagnosis.
There are some common tender points that you should look for when dealing with the diagnosis of fibromyalgia.
1. Base of the neck/skull.
2. Front of the neck.
3. Elbows.
4. Hips.
5. Knees.
6. Lower back.
7. Upper back.
8. Chest.
9. Shoulders.
These points are often referred to as “tender”, but they often don’t exhibit super sharp pain.
Oftentimes, those with fibromyalgia refer to their pain as a deep aching sensation or a “nervy” sensation.
It’s different for each individual, and the other symptoms that can accompany fibromyalgia pain can be troublesome as well.
The following list contains some of the most common symptoms including:
- Chronic fatigue.
- Digestive disorders.
- Brain fog.
- Stomach pain.
- Stiffness.
- Muscle aches.
- Headache.
- Impaired memory.
The list of symptoms appears to be growing as research on this debilitating condition continues to be done.
As these symptoms continue to progress, depression and anxiety are imminent. Individuals that struggle with fibromyalgia often feel that there is no hope.
Those who are still searching for answers may feel overwhelmed at best when they can’t get a “straight answer” from their primary care physician or even a specialist.
Research now points to an interesting fact. Those who are currently suffering from a rheumatic condition may be more likely to have fibromyalgia.
The working list of symptoms is quite similar, and some researchers think that certain rheumatic conditions prime the body for fibromyalgia pain.
According to the National Institute of Arthritis and Musculoskeletal Disease, the following rheumatic conditions may influence the onset of fibromyalgia:
- Rheumatoid arthritis.
- Systemic lupus erythematosus.
- Ankylosing spondylitis.
There are numerous views on what causes fibromyalgia, and researchers are still studying the impact ones environment may have on them developing this condition.
This makes patients that suffer from pain syndromes a target for those who may believe that this isn’t a real condition.
In short, the medical community has deemed fibromyalgia an “arthritis-related condition.”
This isn’t to say that all doctors believe this, but at this time the most common way to define this condition is to associate it with arthritis.
Do you struggle to get up in the morning because you feel stiff?
Do you often feel drained by mid-afternoon?
Do you have chronic widespread joint and muscle pain that cannot be explained?
If you have answered yes to any of these questions, you may be one of the millions that suffer from fibromyalgia.
Outside of your prescription medications and physical therapy, what can you do?
Fibromyalgia Pain-Can PEMF Therapy Give You Relief?
Fibromyalgia isn’t mysterious for those who know they have it.
This painful epidemic is sure to have a lasting impact on those who suffer from it.
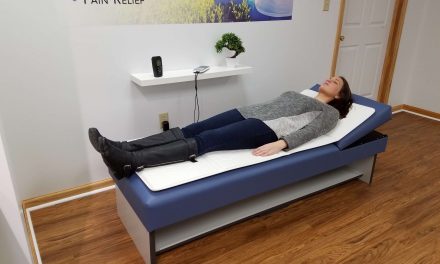
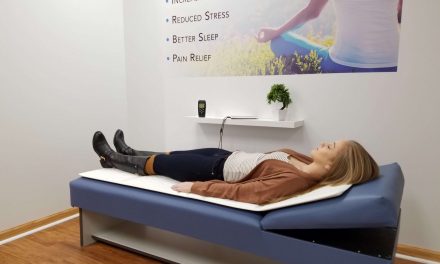
Many who have used PEMF therapy have reported that they have experienced pain relief over the course of a few weeks.
Studies conducted on fibromyalgia patients using PEMF therapy have reflected that using a low-frequency PEMF device has improved function, chronic fatigue, and reduced pain.
This is great news for those who desire to reduce their intake of pain medications or get rid of them altogether.
This therapy is not a replacement for physical therapy or physical activity of any kind, and it’s best to keep moving!
PEMF therapy can help reduce pain because it has been proven to increase blood flow and circulation.
Increasing oxygen levels in tissue is a key component for reducing pain and inflammation, and there are thousands of clinical studies that have been done around the world that prove this.
Many medications have been known to have severe side effects, and they can potentially cause more harm than good.
It is up to you to decide whether or not this therapy is right for you.
Talk with your doctor about your health history. Your doctor knows your medical history best, and they may be able to answer your specific questions about how this could impact your condition and overall health.
If you would like to learn more about how you can access PEMF therapy to reduce your “fibromyalgia pain” at the most affordable rate in North America, please visit www.pemfsupply.com to read about the “easy pay plans” options.