PEMF Therapy for Wound Healing

Wound healing is a complex and crucial process that can greatly impact a person’s overall well-being. Whether it’s a minor cut or a more severe injury, efficient healing is vital for a swift and successful recovery.
One innovative and promising therapy that has gained significant attention in recent years is Pulsed Electromagnetic Field (PEMF) therapy. This non-invasive treatment has shown potential in various medical applications, including pain management, bone healing, and inflammation reduction. In this article, we will explore the fascinating world of PEMF therapy and its promising role in wound healing.
From understanding the basics of PEMF therapy and the wound healing process to learning about the devices and precautions involved, we will delve into how this cutting-edge treatment can become a valuable addition to your wound care routine.
What is PEMF Therapy?
Pulsed Electromagnetic Field (PEMF) therapy is a non-invasive treatment that involves the application of low-frequency electromagnetic pulses to the body. These pulses help to stimulate cellular functions, promoting overall health and wellness. The therapy has been extensively researched and is gaining popularity due to its potential in a wide range of medical applications.
PEMF therapy has its roots in the early 20th century when scientists began exploring the effects of electromagnetic fields on biological systems. The development of PEMF therapy has evolved through several stages, from early experiments with static magnetic fields to the more sophisticated, pulsed fields used today. It was not until the latter half of the 20th century that the therapeutic application of PEMF gained recognition, with numerous clinical studies and trials demonstrating its safety and efficacy.
PEMF therapy works by delivering low-frequency, pulsating electromagnetic fields to the body. These fields penetrate the cells, positively affecting their electrical and chemical processes. PEMF therapy has been shown to increase cellular energy production (ATP), improve blood flow and oxygenation, reduce inflammation, and stimulate the body’s natural healing processes. As a result, PEMF therapy can help to accelerate recovery and promote overall health.
PEMF therapy has been utilized for various medical conditions, including:
- Pain management: Chronic pain, arthritis, fibromyalgia, and migraines
- Bone healing: Fractures, osteoporosis, and bone density improvement
- Inflammation reduction: Autoimmune disorders, sports injuries, and post-surgical recovery
- Neurological conditions: Depression, anxiety, and insomnia
- Wound healing: Accelerating the healing process of acute and chronic wounds
While PEMF therapy is not a cure-all, it can be a valuable complementary treatment for a wide range of health concerns, enhancing the body’s natural ability to heal and repair itself.
Wound Healing Process: The Basics
 Wound healing is a complex, well-coordinated process that can be divided into four stages:
Wound healing is a complex, well-coordinated process that can be divided into four stages:
- Hemostasis: This is the initial stage that occurs immediately after an injury. The body responds by constricting blood vessels and activating clotting factors to form a clot, effectively stopping the bleeding.
- Inflammation: In this stage, the immune system is activated to protect the wound from infection. White blood cells are sent to the site of the injury to eliminate bacteria and debris. Inflammation is a normal part of the healing process but can also cause pain, redness, and swelling.
- Proliferation: During this phase, new cells and blood vessels begin to form, filling the wound and creating a framework for the tissue to regenerate. Fibroblasts (cells that produce collagen) play a significant role in providing strength and structure to the healing wound.
- Remodeling: The final stage of wound healing involves the maturation and remodeling of the new tissue. Collagen fibers are reorganized, and the wound gradually gains strength and elasticity, eventually returning to a more normal appearance.
Various factors can influence the wound healing process, including age, nutrition, general health, blood flow, and the presence of underlying medical conditions such as diabetes. Additionally, factors like infection, poor wound care, and excessive tension on the wound site can lead to delayed or impaired healing.
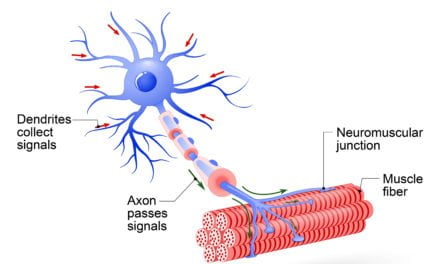
The human body is a complex system of electrical and magnetic fields, with cellular processes relying on the transfer of ions and electrons. These processes are fundamental for cellular communication, growth, and repair. Studies have shown that electromagnetic fields can influence various biological processes, including cell signaling, gene expression, and tissue repair. By applying PEMF therapy, it is possible to stimulate and support the body’s natural healing capabilities at the cellular level.
PEMF Therapy for Wound Healing
PEMF therapy can positively impact the wound healing process in several ways:
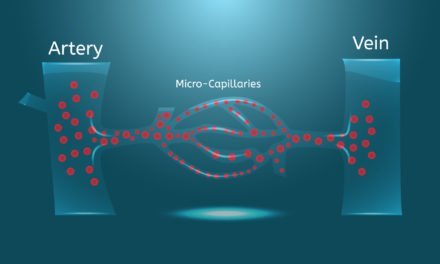
- Increased blood flow and oxygenation: PEMF therapy helps to improve circulation and increase the delivery of oxygen and essential nutrients to the wound site, which is crucial for the healing process.
- Reduced inflammation and pain: By modulating the inflammatory response, PEMF therapy can help to reduce inflammation, swelling, and pain associated with the wound, making the healing process more comfortable for the patient.
- Accelerated tissue regeneration: PEMF therapy has been shown to stimulate cellular processes such as the production of collagen, promoting faster tissue regeneration and improving the overall healing process.
- Enhanced immune response: By supporting the immune system, PEMF therapy can help to reduce the risk of infection and other complications, ensuring a smoother healing process.
Numerous clinical studies[1] and research papers have demonstrated the effectiveness of PEMF therapy in promoting wound healing. These studies have shown that PEMF therapy can improve the rate of wound closure, reduce pain and inflammation, and enhance the overall quality of the healed tissue.
PEMF therapy can be beneficial for a wide range of wounds, including:
- Acute wounds: Cuts, abrasions, burns, and surgical incisions
- Chronic wounds: Diabetic ulcers, pressure sores, and venous ulcers
- Traumatic wounds: Injuries sustained during accidents, sports, or other physical activities
PEMF therapy can be administered by a healthcare professional or used at home with the appropriate equipment. The therapy generally involves placing a PEMF device or applicator near the wound site, with treatment sessions typically lasting between 20 and 60 minutes. The frequency and duration of sessions may vary depending on the severity of the wound and the individual’s response to the therapy. It is essential to consult a healthcare professional for personalized guidance and recommendations.
PEMF Therapy Devices and Equipment
There are various types of PEMF devices available on the market, ranging from portable units for home use to more sophisticated systems found in medical facilities. Some of the most common PEMF devices for wound healing include:
- Portable PEMF devices: These devices are lightweight, user-friendly, and designed for home use, making them ideal for individuals seeking to incorporate PEMF therapy into their wound care routine.
- PEMF mats and pads: These applicators are designed to provide full-body or localized therapy, depending on the size and configuration of the mat or pad. They are versatile and can be used for multiple applications, including wound healing.
- PEMF coils and probes: These applicators are designed to target specific areas of the body and are particularly useful for localized wound healing. They come in various sizes and shapes, allowing for optimal placement near the wound site.

Integrating PEMF Therapy into Your Wound Care Routine
Before starting PEMF therapy, it is essential to consult with a healthcare professional, such as a physician or wound care specialist. They can help determine if PEMF therapy is suitable for your situation and provide personalized guidance on how to integrate it into your wound care routine. Regular follow-ups with your healthcare provider can also help monitor your progress and make any necessary adjustments to your treatment plan.
PEMF therapy should not replace traditional wound care treatments but instead serve as a complementary approach to enhance the healing process. When used in conjunction with proper wound care techniques, such as cleaning the wound, applying appropriate dressings, and managing underlying medical conditions, PEMF therapy can significantly improve wound healing outcomes.
Monitoring your progress while using PEMF therapy is crucial to ensure it effectively supports your wound healing process. Keep a journal or log to record details such as:
- Treatment duration and frequency
- Any changes in wound size, appearance, or pain levels
- Overall improvements in the healing process
- Any side effects or concerns
Sharing this information with your healthcare provider can help them make informed decisions about your treatment plan and provide valuable insights into the effectiveness of PEMF therapy for your specific wound healing needs.

PEMF therapy offers numerous benefits for wound healing, including increased blood flow and oxygenation, reduced inflammation and pain , accelerated tissue regeneration, and enhanced immune response. These advantages make it a valuable complementary treatment to traditional wound care practices, promoting a more efficient and comfortable healing process.
If you or a loved one is struggling with wound healing, consider exploring PEMF therapy as a complementary treatment option. Consult with a healthcare professional to determine if PEMF therapy is right for your situation and to receive personalized guidance on integrating it into your wound care routine.
As research into PEMF therapy continues to grow, we can expect to see further advances in our understanding of its potential applications in wound healing. This expanding knowledge base will help refine treatment protocols and enhance the benefits of PEMF therapy, making it an increasingly valuable tool in promoting optimal healing and overall health.
[1] Callaghan MJ, Chang EI, Seiser N, Aarabi S, Ghali S, Kinnucan ER, Simon BJ, Gurtner GC. Pulsed electromagnetic fields accelerate normal and diabetic wound healing by increasing endogenous FGF-2 release. Plast Reconstr Surg. 2008 Jan;121(1):130-141. doi: 10.1097/01.prs.0000293761.27219.84. PMID: 18176216.
[2] Ross CL, Zhou Y, McCall CE, Soker S, Criswell TL. The Use of Pulsed Electromagnetic Field to Modulate Inflammation and Improve Tissue Regeneration: A Review. Bioelectricity. 2019 Dec 1;1(4):247-259. doi: 10.1089/bioe.2019.0026. Epub 2019 Dec 12. PMID: 34471827; PMCID: PMC8370292.